Nasal prongs seem pretty popular for lots of things these days. So how about their use in kids. There’s a couple of papers out there on its use in the paralysed patient and Dr Andrew Weatherall is here to splice them together.
Isn’t it supposed to be the kids who stuff things up their noses? Have we just seen them do it so often we started wondering about the possibilities ourselves?
Let’s assume not. It’s more a case of people finally getting around to testing things out on kids when they’ve been running with them in adults for quite some time. This time it is THRIVE and that ever so desirable feature of endless maintenance of oxygen saturations while we get around to the ensnorkelling we’ve planned.
In principle that makes plenty of sense. The normal kid is more likely to rapidly desaturate than the normal adult. Physiology is pretty insistent on that. Plus we know people find paediatric intubation tricky so dropping the stress by avoiding the slide of the plethysmograph tone down that digital scale is probably a worthy pursuit.
So how about we look at two papers examining just this issue – does THRIVE employed in the little people stop those saturations from … not thriving??

Australian Angles
First up is this paper published by Humphreys et al, who work out of Brisbane. They did a small RCT on well kids with 24 in the control arm and 24 receiving 100% THRIVE. The kids fell between the ages of 0 and 10 years of age and are reported in the age groups 0-6 months, 6-24 months, 2-5 years and 6-10 years (with a total of 12 in each age range, meaning 6 in the controls and 6 in the THRIVE group within each age group – got it?)
The routine went something like *induction of anaesthesia* –> pre-oxygenation by doing that whole bag-mask ventilation bit –> the mask disappeared and THRIVE was added or nothing was added –> start the stopwatch.
You’ll note that, like the other paper we’ll mention, this is not about patients who are spontaneously ventilating. That’s a completely different thing.
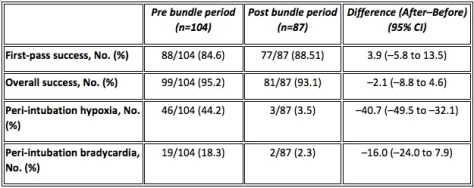
In this group though the period of the saturations staying up was longer. Across the age groups the extension in apnoeic time was 86.8 seconds (0-6 months), 88.7 seconds (6-24 months), 129.5 seconds (2-5 yeas) and 169.2 seconds (6-10 years).
Right, lock it up. Everyone should have nasal prongs. All the time. It’d stop peanuts ending up there too.
Except there’s more pesky nuance in this paper. Like:
1. It’s not for pre-oxygenation
It’s worth noting that the preoxygenation here was all about face-mask ventilation with a good seal. They added THRIVE after that bit and started the clock. This is not entirely surprising because we know that nasal prongs compromise seals in adults and that’s only more likely with kids.
So if you were thinking that you should set up those nasal prongs from the before time zero, you need to think again. THRIVE for preoxygenation is not something tested here, and you shouldn’t assume it’d be better than good face-mask technique.
2. They didn’t test the duration that it worked for apnoea
All they said was it’s ‘more’. ‘Wait,’ you might say, ‘you mean they didn’t test the thing that was the point of study?’
Well not really because the cut-off was ‘twice the previously noted time to desaturation’. So they tested that they could reach the ‘double or nothing’ limit, but didn’t test the full extension. In the THRIVE groups the average saturation when they stopped the clock was 99.6%.
So I guess be reassured that it was likely to be really a heck of a lot of time.
3. Basic things were part of the procedure
For this study there was a lot of basics being done well. Throughout apnoeic oxygenation they weren’t doing things like airway instrumentation, suction, intubation or, I assume, anything much beyond chatting about the weekend and watching the clock. They did jaw thrust, a basic manoeuvre likely to optimise the impact of THRIVE. So maybe we should remember that all those things we are also interested in were not part of the picture.
And Now an Update from the Swiss
What if you didn’t make your cut-off ‘2 times the other cut-off we knew about’? How long could you go?
Well a Swiss crew with no interest in being neutral on the topic I guess have done a study comparing low flow nasal oxygen (0.2 L/kg/min) with THRIVE at either 100% or 30% FiO2 with 20 in each group. And they found … (wait for it…..) 100% THRIVE prolongs apnoea time.
OK there wasn’t much suspense there really.
Except again it was more subtle, and again cut-off matters. They had a cut-off to terminate on the basis of desaturation, but another at 10 minutes (as in ‘it’s 10 minutes and I’m bored let’s stop because those saturations are still great’) and the 3rd cut-off was if the transcutaneous CO2 hit 65 mmHg.
In the THRIVE 100% group no one desaturated, 4 hit 10 minutes and the other 16 had their nasal prongs ditched when they breached the CO2 target. This actually accords with the other paper where they also found that THRIVE doesn’t achieve ventilation and removal of CO2 in kids.
But at the end of this paper you still can’t say how long apnoea might be extended, at least when it comes to those saturations staying up.
Oh, and a couple of other points:
1. Pre-oxygenation was with face-mask ventilation. Again.
Again the nasal option had no role in the preoxygenation phase. They went with face-mask ventilation until the expired oxygen was 90% or above. Then they started the clock with the chosen nasal prong option going.
2. The other airway things done at the time were … none.
Yep. Once again this was just about the oxygen and the stopwatch. Nothing else was going on.

Let’s Think Clinically
So let’s imagine that we’ve actually got that paediatric patient in front of us. Maybe one who needs to get intubated before we get them out of wherever ‘in front of us’ is.
Let’s agree that maintaining oxygenation throughout is a good and noble goal. It’s not the only goal of course. We’d also like to make sure we make good choices around number of attempts, and for some patients (say the patient with intracranial pathology) we need to think about ventilation.
And we don’t have evidence that pre-oxygenation is aided by having THRIVE in place.
So assuming we’re going to do things standard to modern paediatric RSI like face-mask ventilation for a bit before we get going. There is at least a bit of a question about whether THRIVE adds a huge amount.
What it undoubtedly adds is the confidence that saturations will stay up. That is something that lots of practitioners, particularly those not regularly intubating kids would find immensely reassuring.
There is a couple of caveats to keep in mind though.
There’s a risk to be aware of with THRIVE that those saturations staying interminably up might encourage tunnel vision on persisting with intubation when it’s not working out. It’s not too hard to imagine the scenario where the tube hasn’t passed straight down, but those saturations are OK so you persist a bit longer, and a bit longer, and now long enough that the airway is becoming traumatised and suddenly you’ve created a problem.
So this might be a cognitive challenge to have planned for in advance – how do you keep yourself to a limited number of attempts before re-evaluating and going to plan B (or C)? Do you make it a personal process or have others in the crew hold you to a maximum number of attempts or maximum duration of looking?
After all, THRIVE is going to get you to 10 minutes probably. But if you’re still conducting open negotiations with the glottic structures at 10 minutes, oxygenation is not the airway problem that should still be at the front of your mind. While you’re there, you might have to think about re-dosing anaesthetic agents too.
And the other key patient group is that one where intracranial pathology is an issue. Letting the CO2 rise for some patients is not a good plan because your TBI patient (as just one example) doesn’t need those cerebral vessels dilating and the intracranial pressure going up. For those patients, a step back to face-mask ventilation, or potentially placing a supraglottic airway, to re-establish an ability to exchange CO2 is probably a better option.
So THRIVE might be great for some things. But whether it’s clinically better than an approach to the airway where really excellent pre-oxygenation is routine and good practices around face-mask ventilation are established seems like a line ball call.
I mean it’s still way better than a piece of Lego up the nose. But it remains an adjunct to the basic stuff, not a replacement.
Notes:
OK. That first paper is this one:
The second one out of Switzerland is this one:
Did you want something on nasal prongs and seals? You could try this
or this
We’re always interested in other thoughts so feel free to drop a comment.






![What was the big picture again? [via Jarod Carruthers on flickr under CC 2.0 and unaltered]](https://careflightcollective.com/wp-content/uploads/2015/07/trees-copy.jpg?w=474&h=143)
!["Please, go on" says Public Holiday Numbat [unchanged via quollism on flickr under CC]](https://careflightcollective.com/wp-content/uploads/2015/02/numbat-copy.jpg?w=474&h=321)